Why Every Practitioner Tells You Something Different About Your Pain — And What That Means for You
Key Takeaways
If you’ve lived with pain long enough, you’ve probably experienced a familiar and frustrating journey:You visit one practitioner…then another…and anot...
If you’ve lived with pain long enough, you’ve probably experienced a familiar and frustrating journey:
You visit one practitioner…then another…and another…
Each examines the same knee, the same back, the same shoulder —
sometimes even the same MRI —
yet you walk away with completely different explanations.
“It’s inflammation.”
“It’s your posture.”
“It’s an old injury.”
“It’s muscle tension.”
“It’s alignment.”
“This machine will fix it.”
“One adjustment and you’re good.”
Eventually, most people ask:
“Why can’t anyone agree on what’s wrong with me?”
This article is my attempt to explain the pain industry — something I’ve had a front-row seat to for 13 years as the owner and operator of YCK integrated pain clinics.
When you understand how the system works, you can stop chasing the next miracle and start choosing treatments with clarity.
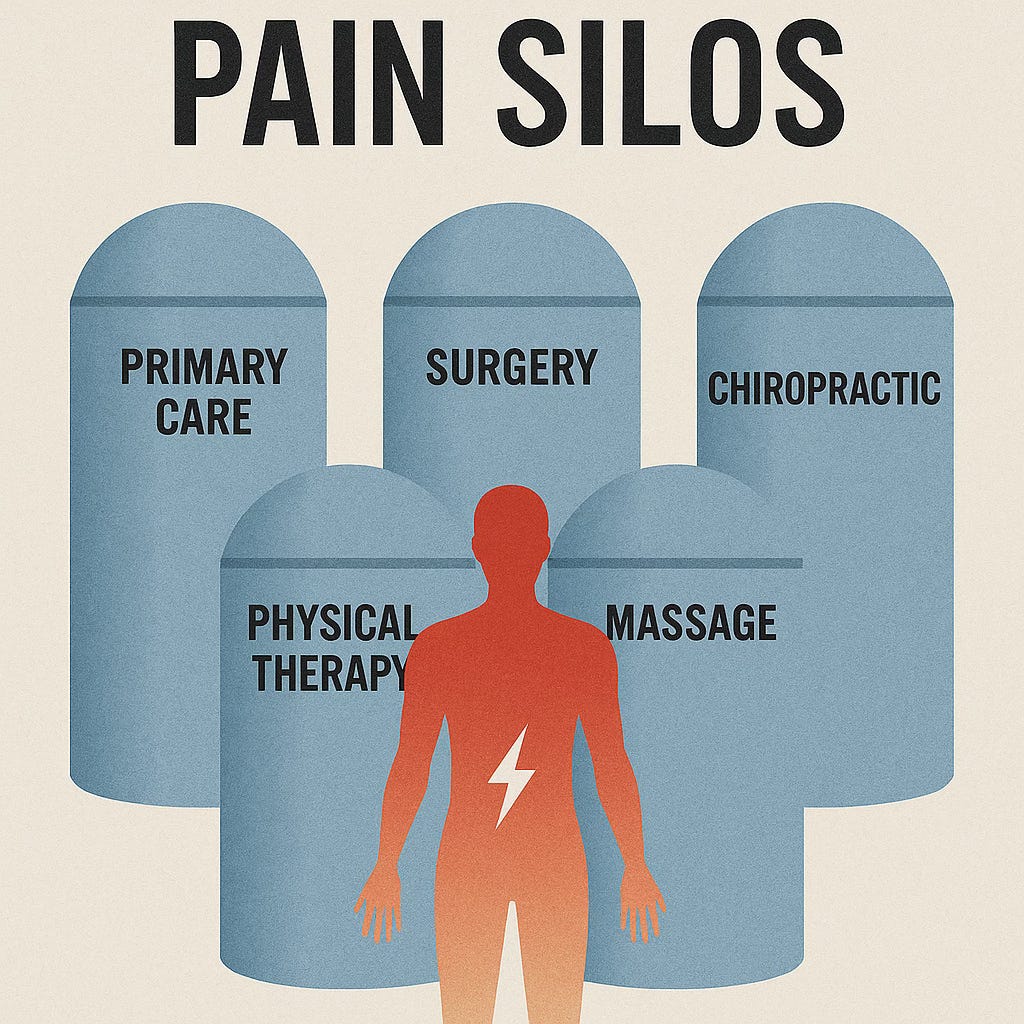
1. Pain is multi-system — but healthcare is single-system
Your pain might feel like it lives in one spot but beneath that pain, multiple systems are involved:
inflammation
muscles and tendons
joints
nerves
movement habits
load tolerance
stress and sleep
These systems interact constantly.
But the moment you see a professional, your pain gets assigned to one lane:
Orthopaedics → structure
Physiotherapy → movement
TCM → inflammation or circulation
Chiropractic → joint mechanics
Sports rehab → load
GP/pharmacist → medication
Each profession focuses on the part they’re trained to fix.
None of them are wrong.
But none of them see the whole picture.
And this is where an old saying suddenly becomes very real:
“To a man with a hammer, everything looks like a nail.”
Every profession brings its own hammer —
exercises, injections, adjustments, herbs, machines, manual therapy —
and naturally sees your pain through the tool they know best.
Not because they’re biased or careless,
but because the system trains each lane to specialise in only one slice of the problem.
This mismatch explains why treatment advice often feels contradictory.
2. The same MRI can mean different things to different people
Patients often believe imaging will give a clear answer. But this isn’t how it works.
A surgeon sees a structural finding.
A physio sees movement dysfunction.
A trainer sees load imbalance.
A chiropractor sees joint restriction.
A TCM practitioner sees inflammatory patterns — described as “heat,” “dampness,” or “qi and blood stagnation” — which map to swelling, stiffness, and impaired healing in modern terms.
Everyone is looking at the same picture but they interpret it through their own tools and training.
People diagnose based on what they are trained to treat. That’s why explanations differ even when the scan does not.
3. Why single treatments sometimes help… and sometimes don’t
This is one of the biggest sources of confusion. You hear from one friend that a PRP injection cured his shoulder pain, and from another that her massage session made things worse. How can the same treatment help one person and not another?
Sometimes a single treatment even feels miraculous:
a steroid injection
PRP
a good manipulation
a deep massage
a stretching routine
a shockwave session
a laser therapy package
a round of NSAIDs
These treatments can help — and they do help many people.
But why do they help one person, yet fail for another?
Because single treatments work best when your pain has a single dominant driver.
Examples:
Steroid injections help when localized inflammation is the main issue.
PRP helps when tendon or tissue quality is the bottleneck.
Manipulation helps when stiff joints are a major factor.
Massage helps when tight, overworked muscles are the main source.
Shockwave therapy can help when tendon healing is the priority.
Laser or ultrasound machines help when superficial inflammation is driving symptoms.
NSAIDs help when inflammatory chemicals are high.
Herbal anti-inflammatory formulas, like the ones we use in our clinics,
help when deep-tissue inflammation and sluggish circulation are part of the picture.
They can make a meaningful difference — but only for people whose pain is driven by that specific pattern.
There is nothing wrong with any of these treatments.
Each one has its place.
But because most chronic pain is rarely caused by a single issue, each treatment ends up addressing only one part of the system.
In reality, pain is usually driven by a combination of factors — inflammation, mobility restrictions, nerve sensitivity, poor load tolerance, habit patterns, sleep and stress, and more.
And that is why short-term relief often fades.
4. Where does surgery fit in?
Surgery can be life-changing — especially for fractures, severe compression, instability, or major tears.
But for common chronic pain:
Spine surgery shows mixed long-term results
Knee arthroscopy often performs no better than physiotherapy for degenerative knees
Rotator cuff repairs depend heavily on tissue quality and rehab
Surgery is valuable but is not the universal answer many hope it will be.
This reinforces the same idea: pain rarely has a single cause.
5. Why “miracle adjusters” look so convincing online
You’ve seen the videos:
A dramatic crack.
A big emotional release.
Instant relief.
The reaction is real —
but it doesn’t tell you what happens over the next three months.
Manipulation can help in some situations. But there is no strong evidence that one adjustment (or even several) cures complex shoulder, knee, or back conditions.
Social media shows the dramatic moment, not the long-term journey.
6. What the research consistently shows
Across decades of studies, a clear pattern emerges:
1. Chronic pain is rarely a single-system problem.
It is almost always a blend.
2. Imaging does not reliably predict pain.
Many people with “bad scans” have no pain;
many with severe pain have normal scans.
3. Treating multiple systems works better than treating one.
Multimodal care repeatedly outperforms single-modality treatments.
4. Behaviour, movement, load, and stress matter deeply.
Pain is physical, but recovery is also behavioural.
This is why no single treatment — machine, injection, adjustment, or medication — solves chronic pain reliably.
7. What real-life recovery looks like when multiple systems are addressed
One thing I’ve learned from years of seeing patients is that real recovery rarely looks dramatic. It’s not a single breakthrough moment.
It’s a steady shift across several systems: pain reducing, movement improving, strength building, and flare-ups becoming less frequent.
A few years ago, when we began integrating physiotherapy with our herbal pain medicine, we ran a simple data exercise in our clinics. It wasn’t anything fancy — no complex trials, no research grants. I just wanted to see, in a structured way, whether the work we were doing in our family clinic was truly helping people.
So our physiotherapists measured what was happening to patients with back, shoulder, and knee pain as they went through treatment.
We tracked three things:
pain levels
range of motion
muscle strength
Across 174 patients, the pattern was consistent:
Pain dropped by 65%–92%
Mobility improved by 53%–155%
Strength increased by 18%–43%
Most of this happened over 8–14 sessions, or roughly a month
This wasn’t because of one technique.
These improvements came from working through multiple parts of the system, step by step — reducing inflammation, improving movement, building tolerance, and gradually changing the habits that were aggravating the issue.
It confirmed something very simple:
When you treat pain as a system, people get better faster and more reliably.
When you treat pain as a single symptom, progress becomes unpredictable.
This small dataset didn’t reveal something new —
it echoed what thousands of studies worldwide already show.
But seeing it happen in real people made the message much clearer.
8. What this means for you
Here is the most honest advice I can offer after years of watching people struggle:
1. You’re not failing treatments.
The treatments are failing to address the whole system.
2. No single practitioner can fix everything.
Each sees one part of the puzzle.
3. Stop expecting a single solution to solve a multi-system problem.
4. Look for logic, not magic.
**5. Choose a recovery path that progresses through multiple systems — not one that promises everything in one go.**
Pain is complex.
Recovery doesn’t have to be.
Once you understand the bigger picture, the world of pain care becomes a lot less confusing — and your next steps become much clearer.
Thank you for reading.
If this piece brought a bit more clarity to the confusing world of pain treatments, I’m glad. There’s so much noise in this space, and if my years inside the industry can help make things feel simpler and more grounded, I’ll keep sharing what I’ve learned.
If someone you know is stuck in the maze of pain options, feel free to pass this along.
And if you’d like to follow along as I write more about pain, recovery, and how the industry really works, you can subscribe below.